Fall Prevention Strategies in Hospitals
Key Takeaways
- Over 650 falls occur in hospitals and mental health units in England and Wales every day.
- Hospital patients are at a higher risk for falls and whether they result in no injury or a severe injury, there are several reasons why falls are serious.
- Research shows that fall prevention programs can reduce the rate of falls.
- Taking universal and patient-specific precautions can help reduce falls and keep your patients safe!
Top Products in This Article
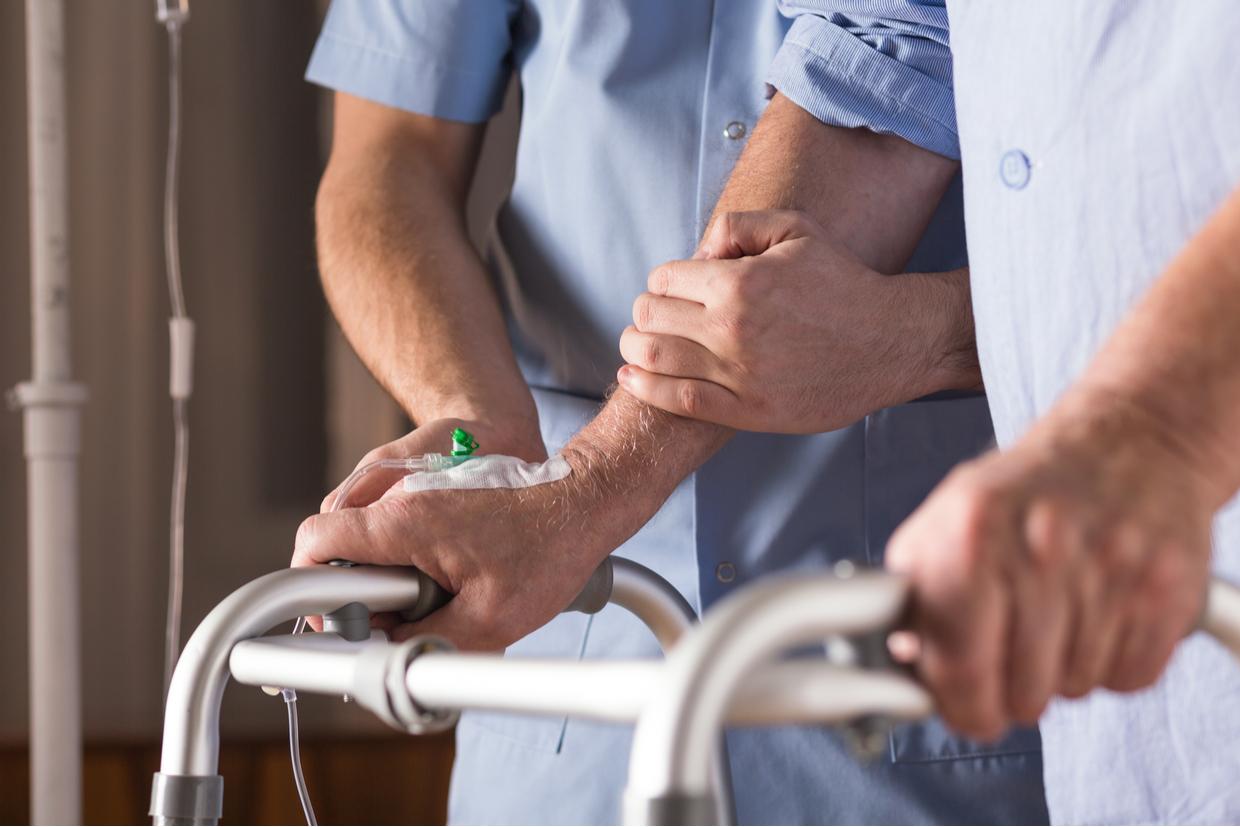
Hospitals are a place where patients come to receive treatment. No medical professional wants to see their patients get hurt while under their care. Fall prevention strategies can reduce your patients’ risk of falling and keep them safe while in the hospital and under your care.
Explore by topic:
Common Questions About Falls in Hospitals
5 Proven Fall Prevention Strategies
Universal Fall Precautions
Patient Specific Fall Prevention Interventions
Patient Education
Fall Prevention Matters
Common Questions About Falls in Hospitals
How common are falls in hospitals?
Around 250,000 falls are reported in hospitals and mental health units in England and Wales every year (that is over 650 a day).1
How many falls in hospitals result in injuries?
In a review done by NHS:1
- 25.5% of falls in hospitals resulted in low harm, requiring first aid, minor treatment, extra observation or medication
- 2% resulted in moderate harm, requiring surgery, a longer hospital stay, or additional outpatient treatment
- 0.5% resulted in severe harm, such as brain damage or disability
- 0.1% resulted in death, where death was the direct cause of the fall
What is the cost of inpatient falls?
The NHS review calculated the average cost of a fall at £2,600, leading to a combined cost to hospitals of reported inpatient falls of around £630 million.1 These estimates do not include the wider costs to the healthcare system such as out-of-hospital rehabilitation services, the need for care/nursing home, and mental health services.
What are the potential savings to reducing falls?
The NHS states that “There is evidence (for example the FallSafe project) that assessments and interventions that take into account a range of factors to identify and treat underlying reasons for falls in hospitals could reduce the incidence by 25-30%. Based on our estimates of the costs of falls, reduction on this scale could mean around 57,000 fewer falls per year and reduce the annual cost of falls by up to 25%.”1
Why are falls without injury also serious?
Even if a patient falls without injury, resulting in a "no harm" fall, it can still have negative effects. These falls can result in fear, distress, and anxiety in patients.
They can also start a negative cycle where patients are afraid to fall, so they restrict their activities to avoid falls. This then causes the patient to lose strength and independence - increasing their risk of falling again.
Why are hospital patients at a higher risk of falling?
Several factors increase the risk of patient falls in hospitals. One factor is that hospital rooms are unfamiliar environments. Another is that some patients are taking medications that may make them dizzy or confused. Additionally, the conditions that lead to patients being in the hospital or the tests and treatments they are undergoing may also leave patients feeling weak or unsteady. These factors, in addition to existing difficulties with mobility and balance, can leave your patients at risk for falls.
Do fall prevention programs work? What does the research say?
Study: Falls prevention in hospitals and mental health units: an extended evaluation of the FallSafe quality improvement project2
Method: Data was collected at baseline and for 18 months from 9 FallSafe units and 9 control units
Intervention: Units in the intervention group were part of a quality improvement project that presented key components of multifactorial assessment and intervention as a care bundle. Components included: Call button in sight and reach, cognitive assessment, asked about fear of falling, history of falls, lying and standing BP, medication review requested, dose of night sedation NOT given last night, safe footwear on feet, and evidence of urine dip-test taken and recorded.
Results: Introducing care bundles led to a significant reduction in fall rates and improved delivery of multifactorial assessment and intervention. The 12 month moving average of reported fall rates showed a consistent downward trend in FallSafe units but not controls.
What fall prevention measures is each member of the Unit Team responsible for?
Clear policies and responsibilities help ensure all fall prevention measures are taken to protect your patients. These roles may vary depending on your staffing configuration.
Nurse
- Complete and documents fall risk screening and assessment
- Document fall prevention practices for individual patients
- Monitor changes in patient’s medical condition
- Report falls to medical provider/physician
- Supervise aides
- Obtain medical orders as needed
- Educate patient and family on fall prevention
- Obtain needed supplies to prevent patient falls (ex. walker, bed alarm, etc.)
Nurse Aide
- Evaluate the safety of the patient's environment during care tasks
- Perform appropriate care plan tasks and reports when they are complete to nurse
- Report changes in patient’s medical condition to nurse
Physician
- Evaluate patient need for specific types of rehabilitation therapy
- Review medications for fall risk and make changes if necessary
- Write orders for specific fall prevention interventions (including activity orders)
Pharmacist
- Review medication of patients that are a high fall risk (based on medication profile) and suggest alternatives meds or dosages to medical providers
Physical or Occupational Therapist
- Make recommendations and trains patient on how to use mobility aids and adaptive equipment
- Provide therapy to patients to improve mobility and ability to perform activities of daily living
- Review activity orders and asks physician to adjust as needed
5 Proven Fall Prevention Strategies
One U.S. hospital reduced its fall rate in their med/surg unit from 10 falls per 1,000 patient days to 2 falls per 1,000 patient days over three years.3 They did this by following a Transforming Care at the Bedside (TCAB) program that targeted patient falls.
These are some of the strategies they used to reduce fall rates at their hospital.
1. Easy Identification of High Fall Risk Patients
- High-risk patients were identified in three ways, so staff could quickly initiate the proper protocols
- They all wore red socks
- High-risk patients also wore armbands
- Visual cues were posted outside of fall-risk patients’ doors
2. Bed Alarms
- Anderson Hospital set their bed alarms so they sounded after one or two seconds instead of ten to reduce the amount of time patients could be out of bed before staff was aware and could intervene.
3. Safety Rounds
- In addition to hourly rounds, nurses conducted twice-daily safety rounds on high-risk patients. During this effective intervention, nurses made sure fall precautions were in place (socks, armband, sign, and alarm).
4. Keeping Patients Busy
- Hospital staff gave patients activities to do to keep them occupied and less likely to get out of bed due to boredom.
- Staff also educated the patient’s family on fall prevention.
5. Provide Safety Companions
- Anderson Hospital increased the number of safety companions who provide continuous monitoring and aid to disoriented patients who were unable to follow direction to help prevent falls.
While all of these solutions may not be the right fit for your hospital, they provide a helpful starting point. Incorporating some of these steps in a universal fall precautions program can help reduce the number of patient falls in your hospital.
Universal Fall Precautions
Universal fall precautions are safety measures that are taken to reduce the chance of falls for all patients, regardless of individual fall risks. Precautions may vary from hospital to hospital, but here’s a list to get you started. These are the components most often see in successful fall prevention trials4:
- Multidisciplinary responsibilities, not solely nurses, but physicians, physical therapists, pharmacists, occupational therapists, and patients and their families too
- Reviewing medication and when appropriate discontinuing the use of medications that are associated with a higher fall risk (psychotropic medication, medication with dizziness or lightheadedness as side effects, etc.)
- Continence management, including frequently offering assistance to use the toilet, commode, or bed pan
- Focusing on preventing, detecting and treating delirium, including testing for urinary tract infections
- Access to mobility aids if necessary
- Provision of safe footwear (not just advice on safe options)
- Early access to physiotherapists and exercise
- Structured staff education from a health professional
- Patient education
Patient Specific Fall Prevention Intervention
In addition to universal fall precautions, it’s important to tailor interventions to individual patient needs. A fall risk assessment can help you identify patients that have a high fall risk and implement patient-specific solutions.
For example, if the patient forgets to call for assistance when walking, using a bed alarms can alert nurses to intervene before the patient falls.

Or if the patient has had a recent fall, discussing how it happened and what to do to prevent a similar fall in the future can help.
These interventions will vary from patient to patient depending on their individual conditions and risk factors.
Patient Education
Patient education is another important part of reducing patient falls, both in the hospital and once patients return home.
Educate patients on why they are at risk for falls and how they can reduce their chance of falls and injuries. Make them aware of the universal precautions that are in place and the steps that have been taken to prevent falls based on their individual risk. A fall prevention handout can be an easy way to start their education.

Hospital staff can re-emphasise key components of the patient’s individualised prevention plan during rounds and rehab sessions (like using the call light instead of getting up alone) to remind patients to follow these interventions.
Fall Prevention Matters
Taking steps to prevent falls keeps your patients safe and can reduce the cost of falls for your hospital. Find additional fall prevention products at Performance Health.
References
- NHS Improvement. (2017). The incidence and costs of inpatient falls in hospitals. National Institute for Health and Care Excellence. Retrieved from https://bit.ly/3ril1H0
- Agency for Healthcare Research and Quality. (2019). Falls. U.S. Department of Healthcare Research and Quality. Retrieved from https://bit.ly/2KuOCKY
- Frances Healey, Derek Lowe, Adam Darowski, Julie Windsor, Jonathan Treml, Lisa Byrne, Janet Husk, Jill Phipps, Falls prevention in hospitals and mental health units: an extended evaluation of the FallSafe quality improvement project, Age and Ageing, Volume 43, Issue 4, July 2014, Pages 484–491. Retrieved from https://bit.ly/3fffDBV
- Becker’s Hospital Review. (2013). 5 Proven Strategies to Prevent Patient Falls. Retrieved from https://bit.ly/2Z28SYC
- Healey, F. (2011). Implementing a Fall Prevention Program. Patient Safety Network (PSNet). Retrieved from https://bit.ly/301oRqZ
Medical Disclaimer: The information provided on this site, including text, graphics, images and other material, are for informational purposes only and are not intended to substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other healthcare professional with any questions or concerns you may have regarding your condition.






 US
US France
France Australia
Australia